The Effect of Morningness-Eveningness on Shift Work Nurses: Sleep Quality, Depressive Symptoms and Occupational Stress
Article information
Abstract
Background and Objective
The purpose of this study was to investigate the effect of morningness-eveningness type on nurses relative to sleep quality, depressive symptoms and occupational stress.
Methods
Data was collected using self-administering questionnaires by 257 three eight-hour randomly rotating shift system nurses at St. Vincent’s Hospital. Questionnaires were composed of baseline demographic data, Korean version of Morningness-Eveningness Questionnaire, Pittsburgh Sleep Quality Index (PSQI), Epworth Sleepiness Scale (ESS), Beck Depression Inventory and Korean Occupational Stress Scale. Kruskal-Wallis H test and analysis of covariance were used to identify significant differences in sleep parameters, depressive symptoms and occupational stress according to morningness-eveningness type.
Results
There was significant difference in Subjective Sleep Quality score (p = 0.018). Post hoc analysis revealed differences between eveningness vs. morningness (p = 0.001) in Subjective Sleep Quality score. There were tendencies in sleep efficiency, PSQI total score and ESS between morningness-eveningness type. However, there were no significant differences in total sleep time, depressive symptoms and occupational stress including eight sub-categories according to morningness-eveningness type.
Conclusions
Eveningness type nurses revealed lower Subjective Sleep Quality and tendency for poor sleep efficiency, poor overall sleep efficiency and more severe daytime sleepiness than other type. However, morningness-eveningness were not decisive factors for total sleep time, depressive symptoms and occupational stress. Short-term medication, workers’ chronotypes consideration and naps before night shifts may be helpful in improving mental health and quality of life for shift nurses, especially for evening shifts.
INTRODUCTION
As technology developed, limitations relative to time spent in workplaces have disappeared. As lifestyles have changed, the numbers of people that work irregular hours are increasing. According to the Second European Survey on Working Conditions in the European Union that was conducted in 2000, only 24 percent of employees worked regular day shifts. Approximately 17 percent in U.S. and 16 percent in Australia worked day and night shifts. From the survey of Ministry of Employment and Labor Work Environment of Korea in 2011, approximately 16 percent were night or shift workers.
Many studies have found that shift work causes various negative side effects. Psychological issues: disruption of biological rhythm, depression and anxiety disorder. Medical issues: cardiovascular diseases, gastrointestinal disease such as dyspepsia, gastric ulcer, back pain and chronic fatigue. Occupational issues: poor performance at work, job dissatisfaction and social isolation [1,2]. Especially, many shift workers suffer from sleep disturbance. This is the reason that shift work schedules cause serious issues in circadian rhythms and sleep-wakefulness patterns [3]. Disturbed circadian rhythm affects human autonomic regulation such as heart rate, blood pressure, and immune and endocrine systems [4].
Compared to daytime or fixed schedules, shift work nurses have psychological, medical and occupational issues as well. For example, they experience issues with disturbed natural human circadian rhythm, low sleep quality, somatic disturbances, decreased heart rate variability and burnout syndrome (emotional exhaustion, depersonalization, and decreased personal accomplishment) [2]. Occupationally they experience errors in patient care such as information loss, less perception of nurse manager ability, leadership and support [5].
Morningness-eveningness indicates that an individual has a preference in diurnal performance, sleep-wake cycle for activity and alertness during the day. These differences are related to individual differences in functioning of the intrinsic circadian system [6]. Morningness-eveningness type influences individual temperament and character. For example, morningness subjects have more patience and harm avoidance behavior while eveningness subjects scored higher in novelty seeking and disinhibition [7]. In addition, morningness-eveningness type may manifest different health behavior patterns. Morningness was significantly related to lower odds of engaging in alcohol consumption, smoking and higher propensity of physical activity [6]. Morningness-eveningness type affects human physiologic homeostasis, too. In stress situations, morningness-eveningness type influences heart rate and rate pressure product (heart rate x systolic blood pressure). For example, eveningness type revealed higher heart rate and rate pressure product in the afternoon at rest and during stress situations [8]. Psychologically, eveningness type experience more depression that may be mediated via circadian effects on the behavioral approach system [9], and eveningness chronotype has cognitive and behavioral issues including attention deficit, hyperactivity and impulsiveness [3]. A study revealed that morningness type students and nurses experience better sleep quality and it was a positive predictor of resilience [10,11], but other studies insist morningness chronotypes experience poor sleep quality [12].
The purpose of this study was to investigate the effect of morningness-eveningness type of shift nurses on their sleep quality, depressive symptoms and occupational stress.
METHODS
Participants and Study Design
Subjects that participated in this study were from a university hospital (St. Vincent’s Hospital, College of Medicine, The Catholic University of Korea). Shift nurses worked as three eight-hour randomly rotating shifts (7:00 am–3:00 pm, 3:00–11:00 pm, and 11:00 pm–7:00 am) 40 hours per week. A cross-sectional study was accomplished with a self-administered, structured questionnaire that contained socio-demographic data, Pittsburgh Sleep Quality Index (PSQI), Epworth Sleepiness Scale (ESS), Beck Depression Inventory (BDI), Korean Occupational Stress Scale (KOSS) and a Korean version of Morningness-Eveningness Questionnaire (MEQ-K). We excluded nurses 1) diagnosed with psychiatric, neurologic or metabolic disorders, 2) taking any psychotropic medications (antipsychotics, antidepressants, benzodiazepines etc.), and 3) worked less than three months. Finally, 257 shift nurses completed questionnaires. This study was conducted June 3–July 14, 2014 and approved by the Institutional Review Board (IRB) of the Catholic University of Korea.
Measures
Korean version of Morningness-Eveningness Questionnaire (MEQ-K) Morningness-eveningness was measured by the MEQ-K [13]. It is composed of a 19-item self-administered scale with questions focusing on habitual waking and sleep periods, preference times of physical and mental behavior, subjective arousal upon awakening and before initiating sleep. MEQ score ranges from 16–86 on morningness-eveningness, with lower scores meaning less morningness. Scores of 41 and below refer to eveningness type, scores of 59 and above refer to morningness type, scores of 42–58 refer to intermediate type [14].
Pittsburgh Sleep Quality Index (PSQI)
PSQI is an effective scale to check sleep patterns and quality in adults. It distinguishes poor from good sleep quality by checking seven measures in the last month: 1) subjective sleep quality, 2) sleep latency, 3) sleep duration, 4) habitual sleep efficiency, 5) sleep disturbances, 6) use of sleeping medications, and 7) daytime dysfunction. The first four questions are open forms and the remaining are 0–3 Likert-type scale. Five or greater score indicates poor sleep quality [15].
Epworth Sleepiness Scale (ESS)
ESS is a questionnaire to check daytime sleepiness, using brief questions. This scale asks the subject to rate their inclination to lapse into sleep on a scale from 0 to point 3 for eight various situations that most people participate in during their ordinary lives. From 0 to 9 is normal while more than 10 point means daytime over sleepiness [14].
Beck Depression Inventory (BDI)
BDI consists of a 21-question, multiple selecting self-administered inventory, that is a widely used psychometric scale for assessing depression severity [16].
Korean Occupational Stress Scale (KOSS)
KOSS is composed of 43 questions in eight sub categories 1) physical environment, 2) job demand, 3) insufficient job control, 4) interpersonal conflict, 5) job insecurity, 6) organizational system, 7) lack of reward, and 8) occupational climate. KOSS is a validated scale of the national study for development and standardization of occupational stress in Korea to assess occupational stress standards [17]. Total stress scores and eight sub categories were standardized by 100 points.
Statistical Analysis
Statistical analyses were performed with the Statistical Package for Social Sciences software (SPSS, version 21.0; SPSS Inc., Chicago, IL, USA). Kruskal-Wallis H test was used to measure potential differences between morningness-eveningness chronotype for all continuous demographic variables. To evaluate group differences between morningness-eveningness chronotype and dependent variables (sleep parameters, BDI, Occupational Stress Scale), we used analysis of covariance that statistically adjusts covariates. If there was a significant difference, post hoc analysis with Bonferroni’s correction was applied. All statistical analyses used a two-tailed α level of 0.05 for defining statistical significance.
RESULTS
Demographic and Sleep Data
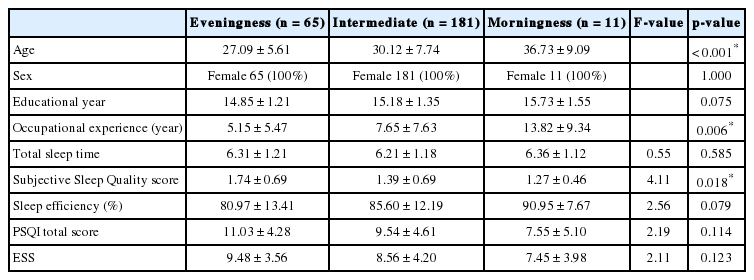
Table 1 shows basic demographic and sleep data in our three different groups. This study revealed 65 (25.3 percent) of shift nurses were in the eveningness group, 181 (70.4 percent) in the intermediate group, and 11 (4.3 percent) in the morningness group. All participants were female. Age was different between groups and statistically significant (27.09 ± 5.61 vs. 30.12 ± 7.74 vs. 36.73 ± 9.09, p < 0.001). Educational year differences were not statistically significant. There was significant difference in occupational experience years between groups (5.15 ± 5.47 vs. 7.65 ± 7.63 vs. 13.82 ± 9.34, p = 0.006).
There was significant difference of Subjective Sleep Quality that is one of PSQI subscales (1.74 ± 0.69 vs. 1.39 ± 0.69 vs. 1.27 ± 0.46, p = 0.018). Post hoc analysis revealed differences between eveningness vs. morningness but between eveningness vs. intermediate and intermediate vs. morningness did not reveal significant differences. Morningness-eveningness type was not associated with total sleep time. Sleep efficiency was higher in morningness type but statistically insignificant. Eveningness type has poorer sleep quality and more severe day time sleepiness, but was statistically insignificant.
Depression and Occupational Stress
Table 2 shows group comparison analysis of the Depression and Occupational Stress (including eight sub categories). Depression evaluated by BDI was insignificant between groups. Difference of total occupational stress between groups was insignificant (50.35 ± 9.94 vs. 50.15 ± 9.80 vs. 53.92 ± 10.42, p = 0.388). Morningness-eveningness type did not reveal association with stress due to physical environment, job demand, insufficient job control, interpersonal conflict, job insecurity, organizational system, lack of reward, and stress due to occupational climate.
DISCUSSION
In this study, we revealed the effect of morningness-eveningness type of shift nurses on their sleep quality, depressive symptoms and occupational stress. As we age, we become more morningness types. It is because our sleep cycle is steadily advanced by circadian system as we age, and people become accustomed to waking early and working during the early hours [18]. Sleep is a parameter that is markedly impacted by shift work [19]. After night shifts, people usually sleep during the day but their daytime sleep quality is poorer compared to typical night time sleep [20]. From our study, total sleep time was statistically insignificant according to morningness-eveningness type. The World Health Organization recommends 7–8 hours of sleep for adults to recover from physical and psychiatric fatigue. However, Koreans have the least sleep time in OECD countries (Korean adults’ mean sleep time was only 6.5 hours) [21]. In this study, total sleep time of shift nurses was an average of 6.3 hours but morningness-eveningness type was not a decisive factor for total sleep time. Although total sleep time was insignificant between groups, Subjective Sleep Quality score revealed significant differences between morningness-eveningness chronotype. Post hoc analysis indicates that morningness type has better Subjective Sleep Quality compared to eveningness type. Previous studies have validated that various kinds of shift workers experience depressive symptoms [9,22]. Mean BDI score of subjects was more than 10 points, indicating mild depression but there were insignificant differences between groups.
Shift nurses have moderate occupational stress that was measured by KOSS but it did not reveal significant differences between groups. Shift nurses experience stress due to physical environments such as physical burden, risk and pollution. They have severe stress due to job demand including time pressure, excessive occupational responsibility and workload. When the stress due to job demand score is more than 70, immediate reduction of work load is recommended. Shift nurses experience moderate stress due to insufficient job control conditions including low decision-making rights and task predictability. However, occupational stress due to physical environment, job demand and insufficient job control were not associated with morningness-eveningness type. Participants revealed relatively low stress due to interpersonal conflict and job insecurity. It is because St. Vincent’s Hospital has a relatively strong support system, friendly workplace culture and stable employment system, but interpersonal conflict and job insecurity were not associated with morningness-eveningness type. Shift nurses have moderate stress due to organizational systems. Reward systems consist of financial payment, mutual respect, inner motive and skill development opportunity. These two measures (organizational system and lack of reward) were not associated with morningness-eveningness type. Stress due to occupational climate means that workers suffer from inflexible decision-making processes, workplace sexual discrimination and unwanted official dining after work hours. Subjects experienced moderate level occupational climate stress.
There are limitations of this study. First, it was conducted in one university nurse population with a self-administered questionnaire, so it may have biased responses from participants. Second, in U.S., male to female ratio of nurses is 1 to 9.5 or 8.1 percent, but all subjects of this study are females that work in the same hospital with small sampling size. Morningness type ratio was too limiting (4.3 percent) compared to other studies (range from 16.4 percent–30.5 percent) [7,23]. Therefore, generalizations should be considered with precaution. Third, this was a cross-sectional study, and therefore it was difficult to find causal relationship. Issues of health caring shift workers were not rare and eventually compromised service quality including patients’ safety. For shift nurses, eveningness chronotypes were vulnerable to shift work, especially sleep (Subjective Sleep Quality score). Poor Subjective Sleep Quality could cause various problems including day time sleepiness [24]. Naps decrease sleep pressure and reduce next day slow wave activity, so taking a nap before night shift work may be helpful to eveningness types [23]. Flexible and adaptive sleep strategies may also be helpful in decreasing sleep-wake cycle dysregulation [25]. Modafinil may be helpful for increasing awakening during night work and may be effect in modifying disturbed circadian rhythm [26,27]. More than 12-hour shift work was associated with poor job performance and lower satisfaction [28]. Therefore, limiting shift work time is necessary for shift workers’ wellbeing and job efficiency. In addition, when organizing shift work, workers’ chronotypes should be considered as well. Eveningness types usually suffer from daytime sleepiness, so regular breaks are necessary to increase work efficiency. Further studies for managing occupational stress, improving sleep quality and overall well-being with larger populations are needed for shift workers.
Notes
Conflicts of Interest
The authors have no financial conflicts of interest.