Exploring the Intersection of Narcolepsy and Attention Deficit Hyperactivity Disorder: Similarities, Differences, and Clinical Implications
Article information
Abstract
Narcolepsy and attention deficit hyperactivity disorder (ADHD) are distinct neurobiological conditions characterized by overlapping symptoms, including excessive daytime sleepiness and cognitive dysfunction. Despite their differences in etiology and pathophysiology, recent studies have highlighted a potential association between the two disorders, with a significant prevalence of ADHD symptoms observed in narcolepsy patients. This narrative review explores the similarities and differences between narcolepsy and ADHD, focusing on their shared symptomatology, neurobiological mechanisms, challenges in diagnosis, and treatment implications. While both disorders exhibit disruptions in dopaminergic and noradrenergic neurotransmitter systems, differential diagnosis remains challenging due to overlapping clinical presentations. Polysomnography findings, such as appearance of sleep onset rapid eye movements in narcolepsy patients, provide important distinctions that enable accurate diagnosis. Treatment strategies often involve stimulant medications for symptom management; however, nonpharmacological interventions, such as cognitive behavioral therapy, have been shown to have the potential to improve patient outcomes. Clinicians must consider the possibility of coexisting narcolepsy in ADHD patients and vice versa to ensure appropriate treatment selection and optimal patient care. Further research is needed to refine diagnostic criteria, elucidate the complex interplay between the two disorders, and develop personalized therapeutic approaches. A multidisciplinary approach involving sleep specialists, neurologists, psychiatrists, and psychologists is essential to address the diverse biopsychosocial needs of patients with concurrent narcolepsy and ADHD.
INTRODUCTION
Narcolepsy is a chronic sleep disorder that manifests with excessive daytime sleepiness (EDS), with or without sudden muscle weakness (cataplexy), sleep paralysis, hypnagogic and hypnopompic hallucinations, and disrupted nighttime sleep [1]. According to the International Classification of Sleep Disorders-Third Edition (ICSD-3), narcolepsy is classified into two primary types: narcolepsy type 1 (NT1) and narcolepsy type 2 (NT2) [2,3]. The key distinguishing criterion between these two types lies in the presence of cataplexy or neuropeptide hypocretin-1 levels in the cerebrospinal fluid (CSF). Since both NT1 and NT2 shared core symptoms like EDS and nighttime sleep disturbance, patients with NT1 and NT2 have reduced academic performance and quality of life [4]. Notably, patients with narcolepsy suffer from psychiatric disorders including major depressive disorders, general anxiety disorders, and attention deficit hyperactivity disorder (ADHD) as comorbidities [5]. As reported in one systematic review, the prevalence of ADHD symptoms was over 30% in narcolepsy patients; therefore, when treating narcolepsy patients, the possibility of ADHD comorbid should be considered [6].
ADHD, characterized by inattention, impulsivity, and hyperactivity, is one of the most common neurodevelopmental disorders. The prevalence of ADHD in children is between 2% and 7% [7], and in nearly 55% of the patients, ADHD persists into adulthood [8]. Children with ADHD may suffer from EDS and other sleep problems than those without [9]. Especially, in a previous study, adults with ADHD symptoms had a history of childhood narcolepsy [10], which makes it difficult to differentiate between ADHD and narcolepsy. In addition, psychopharmacological treatments for ADHD are similar to those of narcolepsy [11], so attention to the interrelationship between these two diseases is needed.
There are several literatures on the correlations between ADHD and narcolepsy [6,12-15]. Two recent systematic reviews suggested that patients with narcolepsy had a higher prevalence of ADHD symptoms than the control group [6,15]. In one study in Norway, patients with narcolepsy who had unmedicated postpandemic influenza A (H1N1), which found correlations with narcolepsy prevalence before [16], had more ADHD symptoms than patients with medicated narcolepsy [12]. However, since most of these studies are questionnaire-based or cohort database-based studies, there was a limitation in that it was difficult to find a pathophysiological connection.
This mini-narrative review aimed to find correlations and discrepancies between narcolepsy and ADHD, with a focus on overlapping symptoms, challenges in diagnosis, and recent research findings. By exploring the similarities and differences between the two disorders, we aimed to contribute to a comprehensive understanding of their coexistence and give a future direction for researchers.
PATHOPHYSIOLOGY AND DIAGNOSIS OF ADHD AND NARCOLEPSY
The etiology of ADHD varies and has been associated with genetic, perinatal, and environmental factors [17]. In genetic factors associated with ADHD, neurotrophins, including brainderived neurotrophic factor (BDNF) and dopamine transporter, have been associated with ADHD [17]. In addition, patients with ADHD have shown a general reduction in brain size, particularly affecting the prefrontal cortex, corpus callosum, caudate nucleus, and globus pallidus, and deficient dopaminergic and noradrenergic transmission in different brain circuits have been linked to several symptoms [18]. The dopaminergic system and noradrenergic system, some of the most studied neurotransmitter systems, are associated with ADHD, and dopamine transporter is the main target of two main categories of ADHD pharmacologic treatments; stimulants [19] and non-stimulants, including viloxazine, which was recently approved for ADHD [20].
On the other hand, the pathophysiology of NT1 is associated with hypocretin (Hcrt), also called orexin [1]. Hcrt-1 and Hcrt-2 (also known as orexin-A and orexin-B) are neuropeptides related to the arousal system, and they play a significant role in regulating the sleep–wake cycle, the reward system, neuroendocrine, and autonomic systems [21]. They activate neurons in which norepinephrine and dopamine are synthesized, exerting enduring effects that facilitate the sustenance of wakefulness throughout the day [21]. Hcrt suppresses rapid eye movements (REM) sleep, so when it decreases, it can trigger the component of REM sleep leading to symptoms like sleep paralysis, cataplexy, and hypnagogic hallucination [1,21]. The precise mechanisms for triggering the degeneration of Hcrt neurons are not fully understood; however, there is widespread consensus that NT1 is likely an autoimmune disorder. The most important evidence supporting NT1 as an autoimmune disorder is an association with the HLA allele, HLA-DQB1*06:02, which are T cell receptor gene variants and polymorphisms that are also correlated with other autoimmune diseases [22]. In contrast, NT2 is recognized for its comparatively weak association with HLA-DQB1*06:02 and Hcrt [22,23], and the underlying pathophysiology of NT2 remains unclear. In addition, there is controversy on the diagnosis of NT2, given that 10% of NT2 patients are subsequently rediagnosed as NT1 as shown in the future [1,22,23].
The existing diagnostic criteria for ADHD, rooted in subjective reports and clinical presentations, demonstrate high sensitivity, making it challenging to discern definitive pathology from ordinary variations [24]. In recent studies, researchers suggested that the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) criteria lead to over-diagnosis, with lower clinical thresholds than the previous DSM criteria [25]. Assessment tools like Conners’s adult ADHD rating scale [26] and adult ADHD rating scale [27] are also used to diagnose ADHD; however, recent studies showed that these tools have low specificity [27]. Considering false-positive rates, researchers suggested that semi-structured interviews or neuropsychological tests can increase the validity of diagnosis when evaluating ADHD [28].
ICSD-3 describes two types of narcolepsy, NT1 and NT2 [2]. NT1 diagnosis is established by cataplexy, two or more sleep onset rapid eye movement periods, sleep latency of ≤8 min on a multiple sleep latency test (MSLT), and/or CSF hypocretin-1 concentration of ≤110 pg/mL or <1/3 of mean control values. NT2 diagnosis is established by the absence of cataplexy, CSF hypocretin-1 concentration not measured or >110 pg/mL or >1/3 of mean control values, hypersomnolence, and/or MSLT findings not better explained by other causes [2].
OVERLAPPING SYMPTOMS AND NEUROBIOLOGICAL MECHANISMS OF NARCOLEPSY AND ADHD
Previous studies suggested that ADHD and sleep effects occur in both directions [29]. In other words, sleep disturbance can cause ADHD symptoms like inattention and hyperactivity [29], and conversely, ADHD patients can experience sleep disturbance [30]. From this perspective, ADHD is often associated with several comorbid sleep disorders. For instance, approximately 44% of individuals affected by ADHD experience periodic limb movement disorder [31,32]. Also, ADHD patients, especially children, commonly report obstructive sleep apnea [33]. Subjective sleep issues are reported in 25% to 55% of cases, while sleep phase and circadian sleep-wake rhythm disorders are prevalent in 73% to 78% of individuals with ADHD [34,35]. Notably, one meta-analysis suggested that children and adolescents with ADHD presented significantly increased sleep latency and decreased sleep efficiency in actigraphy, but not in polysomnographic measures [36]. In addition, in a previous study, compared to controls, patients with ADHD had significantly higher slow-wave activity in sleep encephalography (EEG) during their early childhood; however, it was lower during their adolescence [37]. While polysomnography shows a decrease in slow-wave sleep in narcolepsy patients, the two disorders may share a similar biological background [38].
When considering attention from the perspective of narcolepsy, one functional magnetic resonance imaging study suggested that patients with narcolepsy had impaired executive function compared to healthy controls [39]. They found that when narcolepsy patients performed a sustained attention task, activities in cingulo-opercular, frontoparietal, arousal, motor, and visual networks, which are correlated with executive function, their performance was lower than that of the control group [39]. As executive functions include regulating performance, response inhibition, and working memory, which are related to attention [40], in patients with narcolepsy the function of attention could be affected. These results are the same as those in the previous studies using the attention task, in which narcolepsy patients showed no significant difference in the number of errors compared to the control group, but the response time was slower [41]. Another study also suggested that narcolepsy patients with REM sleep behavior disorder had higher impulsivity and low objective attention profile compared with the control group [42].
A genetic background study conducted in Japan also found that ADHD and narcolepsy could share common biological mechanisms associated with dopamine signaling, immune system regulation, glial cell function, and iron homeostasis on gene-set enrichment analysis [43]. Other studies explained the hypothesis of the association of these two diseases with neurotransmitters, based on the fact that both diseases are related to dopaminergic and noradrenergic systems, so both are treated using methylphenidate and modafinil [1,7,15,20]. Dysfunction within these neurotransmitter systems can lead to disturbances in executive functions, including attentional control, inhibitory control, and working memory, commonly observed in both narcolepsy and ADHD [7,15,44].
PREVALENCE OF ADHD IN NARCOLEPSY AND DIFFERENTIAL DIAGNOSIS CHALLENGES
The potential association between ADHD and narcolepsy has recently attracted attention [6,9,15]. Two systematic reviews suggested that the prevalence of ADHD symptoms was higher in narcolepsy patients compared with normal control [6,15]. One systematic review included five studies examining a total of 328 patients suggesting that the comorbidity of ADHD symptoms in narcolepsy patients was 33.0% [6]. Recently, another study based on 10 studies with 839 patients suggested that the total comorbidity of ADHD in narcolepsy was 25% [15]. In particular, this study emphasized that the comorbidity of ADHD symptoms was significantly higher in NT2 than in NT1 [15]. Another study in China reported important prognosis results, adolescents with NT1 had high comorbidity of ADHD (28.8%) and patients who had comorbid ADHD were associated with increased levels of mood disorder and lower quality of life [45]. These results give evidence for the association between NT1 and ADHD, but the results of other studies were inconsistent with those of the above studies. One recent systematic review has also suggested that ADHD is more frequently comorbid in NT2 than in NT1 [13,15]. They also reported the possibility that ADHD is a subtype of NT2, considering the heterogeneity and variety of NT2 [13].
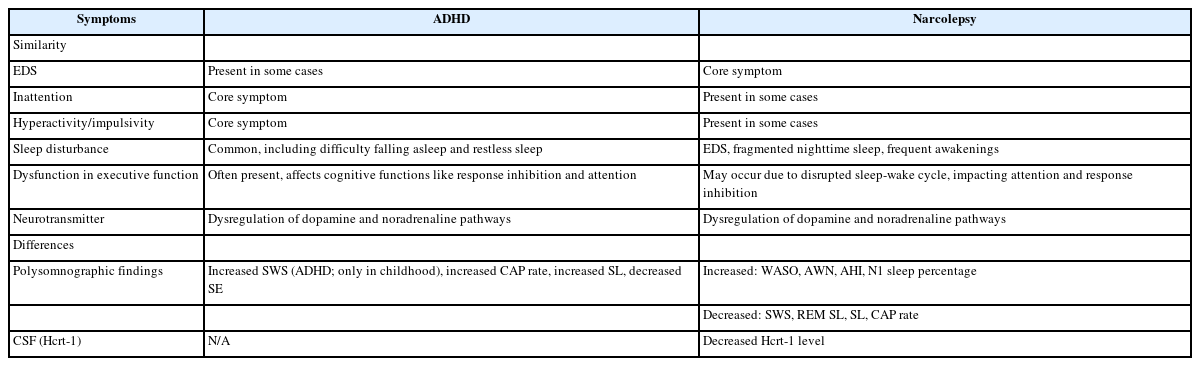
Owing to the similarities between narcolepsy and ADHD, distinguishing between the two disorders could be challenging due to overlapping symptoms. Table 1 shows the similarities and differences between these two diseases. One cohort study revealed that the first symptoms of patients’ narcolepsy, which led to the first hospital visit were EDS, inattention, and decreased academic performance [46]. These symptoms are similar to those of ADHD [7], and ADHD patients have sleep problems [47], which makes it difficult to distinguish between these two diseases. On the other hand, considering the high coexistence rate of attention problems in narcolepsy [6,12,13] and the comorbidity of sleep problems in ADHD [9,47-49], the possibility of the coexistence of the two diseases or delayed diagnosis of narcolepsy should be carefully considered. According to a cohort study, it takes an average of 3.6 years from the onset of narcolepsy symptoms to the diagnosis of narcolepsy, with 19.2% of patients who had childhood onset symptoms and 12.3% of patients who had adult onset symptoms being misdiagnosed as ADHD at the first diagnosis [46]. Considering the impact of narcolepsy treatment on patients’ quality of life, these diagnostic delays can affect patients’ quality of life [50]. Therefore, before diagnosing ADHD, clinicians may need to understand and consider the possibility of narcolepsy [46].
However, there are also differences between the two diseases. In polysomnography, narcolepsy patients had increased wake time after sleep onset, awakening numbers per hour, apnea/hypopnea index, and N1 sleep percentage, decreased slow wave sleep, REM sleep latency, sleep latency, and cyclic alternating pattern (CAP) rate [38]. On the other hand, polysomnography in ADHD patients only showed increased slow-wave sleep in childhood and increased non-REM sleep CAP rate [37]. This difference may be due to Hcrt, which regulates REM sleep, as evidenced by CSF Hcrt-1 level reduction in NT1 [21].
TREATMENT AND CLINICAL IMPLICATIONS
Because shared symptomatology makes it difficult to differentiate between narcolepsy and ADHD diagnosis, clinicians should select appropriate treatment strategies for better patient outcomes. However, stimulant medications like methylphenidate and modafinil are commonly prescribed for both ADHD symptoms and EDS in narcolepsy [15,44]. In addition to stimulant medication; however, given the potential disparity in medication for each condition, such as pitolisant for treating EDS symptoms in narcolepsy, 5-HT3 antagonist/inverse agonist [51], and nonstimulant medication like viloxazine for ADHD [20]. Moreover, previous research indicate that nonpharmacological interventions for ADHD, such as cognitive behavioral therapy (CBT), when combined with pharmacotherapy, contribute to enhanced patient quality of life [52]. Similarly, studies suggested that nonpharmacologic treatments such as CBT and physical activity for improving EDS and cognitive dysfunction had significant effects in patients with narcolepsy [53]. Therefore, it will be important for clinicians to examine the presence of ADHD symptoms in patients with narcolepsy and to consider the possibility of narcolepsy in ADHD patients.
CONCLUSION
Further research is warranted to elucidate the intricate interplay between narcolepsy and ADHD and refine diagnostic criteria to facilitate accurate differential diagnosis. Longitudinal studies examining the natural course of the two disorders and their comorbid presentations are crucial for delineating distinct phenotypic profiles and prognostic implications. Moreover, advances in neuroimaging techniques and biomarker discovery hold promise for identifying novel therapeutic targets and personalized treatment approaches. Clinicians must adopt a multidisciplinary approach encompassing sleep specialists, neurologists, psychiatrists, and psychologists to provide comprehensive care that will address the complex biopsychosocial needs of patients with concurrent narcolepsy and ADHD.
Notes
Availability of Data and Material
Data sharing not applicable to this article as no datasets were generated or analyzed during the study.
Author Contributions
Conceptualization: Seung Chul Hong, Sung Hoon Yoon. Data curation: Sung Hoon Yoon, Young-Chan Kim. Formal analysis: Sung Hoon Yoon, Seung Chul Hong. Methodology: Sung Hoon Yoon, Yoo Hyun Um, Seung Chul Hong. Supervision: Tae Won Kim, Ho Jun Seo, Jong-Hyun Jeong, Yoo Hyun Um, Seung Chul Hong. Validation: Tae Won Kim, Jong-Hyun Jeong, Yoo Hyun Um, Seung Chul Hong. Visualization: Sung Hoon Yoon. Writing—original draft: Sung Hoon Yoon. Writing—review & editing: all authors.
Conflicts of Interest
Seung Chul Hong, a contributing editor of the Sleep Medicine Reseasrch, was not involved in the editorial evaluation or decision to publish this article. All remaining authors have declared no conflicts of interest.
Funding Statement
None
Acknowledgements
None