AbstractBackground and ObjectiveExcessive daytime sleepiness (EDS) is an important public health issue requiring adequate screening and management to avoid such harmful consequences. The study aimed to assess the prevalence and risk factors of EDS in the perinatal period.
MethodsInstitution-based cross-sectional study was carried out in selected public health institutions of Ethiopia on systematic selected 362 women during perinatal period. We used a validated Epworth daytime sleepiness tool to collect data. Epi-InfoTM 7 and SPSS version 26 were used for data entry and analysis, respectively. Bivariable and multivariable binary logistic regression analyses were conducted to determine the associated factors.
ResultsThe prevalence of EDS was 16.6% (95% CI: 12.6–20.7). Excessive pregnancy-related concern (adjusted odds ratio [AOR] = 0.232, 95% CI: 0.087–0.621), having depression symptoms (AOR = 8.045, 95% CI: 3.375–19.174), anxiety symptoms (AOR = 4.905, 95% CI: 2.083– 11.550) and having a chronic medical illness (AOR = 5.441, 95% CI: 2.273–13.021) were the factors associated with EDS.
INTRODUCTIONThe perinatal period is a time characterized by several physical and emotional changes. During the perinatal period several structural, hormonal and other body chemicals were changed [1], as a result, women were highly vulnerable to emotional and psychological conditions such as sleep disturbance, mood, anxiety and others that influence the mother and child’s development and health [2,3]. It is also characterized by a decrease in physical structure and strength, a feeling of fatigue, breastfeeding, and role transition, which results in a painful effect on the mothers and their child’s health [2-4].
Sleep is a natural, temporal state of mind, in which an individual becomes physically inactive, has lower body function and is unaware of the surrounding environment [1,5]. Physical, psychological, social and hormonal changes during the perinatal period disturb women’s sleep patterns [4,6,7]. Sleep problems in the perinatal period, especially during pregnancy, are common health problems [6,7]. A recent study showed that 76%–97% and 33.2% of women experienced sleep problems in the antenatal and postnatal periods, respectively [3].
The common form of sleep disorder during the perinatal period is hyper somnolence (waking up in the middle of the night, daytime sleepiness, and sleeplessness) or insomnia, sleep-related movement disorders, and sleep-related breathing disorders [8-10]. Excessive daytime sleepiness (EDS) is a common public health concern and is a direct and/or indirect predictor for other sleep-related and non-sleep-related problems. It is also characterized by difficulty staying awake and alert during the major waking episodes of the day [4,7].
EDS is one of the most frequent sleep complaints in various populations [11,12], and highly associated with disability [11], and also leads to a deleterious impact on health [13,14]. EDS plays a major role in influencing the mental and physiological health status of women [3,4,7]. The prevalence of EDS among different study populations was 49% in the USA [15], 11% in Canada [16], 13.2% in Korea [17], 18.9% in Japan [11], 33% in France [18], 13.6% in Australia [19], and 31.07% in Ethiopia [13].
Various study revealed that younger age [20-23], high school educational level [24] unemployment status [25], respiratory comorbidity [16], having depression symptoms [21,23,26-29], low body mass index, high degree of workload [22], the presence chronic medical illness such as diabetes mellitus [24,30], being pregnant [25], use of selective serotonin reuptake inhibitors [23], having anxiety symptoms and substance use like smoking [28] were factors associated with EDS.
Sleepiness affects performance differently. It is linked to sleepy periods happening while performing tasks that need a lot of concentration, such driving a car, and may create obvious disturbances in social or occupational functioning [19]. Sleepiness also causes a broad range of neuropsychological deficits, including cognitive dysfunction, depression, and irritability [13,19,20,31]. Additionally, this degree of impairment in women during perinatal time may result in clear wakefulness, morbidity, accidents on herself and their child, and a variety of job and social situation limitations [32].
Permanent EDS can cause deprived health status [11], poor quality of life [16], increased risk of accidents [11], limit productivity and social connections [33], psychological or mental distress [4,7], and poor academic performance. In Ethiopia, there is a scarcity of studies concerning EDS among women and no study was conducted among women in the perinatal period. So, the current study intended to determine the magnitude of perinatal EDS and identify associated factors among women in Ethiopia.
METHODSParticipantsA total of 362 women was determined using a single population proportion formula with the following assumptions; the magnitude of EDS (prevalence = 31.07% [13]), 95% confidence interval (CI), the margin of error (d) = 5% and adding 10% nonresponse rate. The researcher recruited the study respondents using a systematic random sampling method for a period spanning from March, 1, 2022, to June, 15, 2022. Since the total number of women that get a perinatal service per month was 1430 and the number of required test subjects was 362, a sampling interval of four was used as the constant difference between subjects. The first starting number of each study site was picked randomly using the lottery method from the registration counter. Inclusion criteria for the enrolling women were age of ≥ 18 years, having regular antenatal care and postnatal care follow-up, as well as women who would come for delivery during the study period if they were volunteers. Women who are unable to hear or speak and the severely ill who did not fully complete the questionnaires were excluded from the study.
Study Design and Data CollectionA cross-sectional study was carried out with a structured interviewer-administered questionnaire to obtain socio-demographic information including residence, age, educational level, occupation, chronic diseases, including hypertension, diabetes, tuberculosis, and other relevant associated information, from the respondents. Through data collection and processing, complete confidentiality was obtained from unnamed questionnaires. Before starting the questionnaire, written consent was obtained from every participant.
Perinatal EDS was assessed by using the Amharic (a regional language that is widely understood in the society) translated version of the Epworth daytime sleepiness scale, which was validated in Ethiopia [32] with a reliability test of 0.725, which is acceptable [13] and contains eight situations commonly encountered in daily life. The total score of the ESS ranged from 0 to 24. The higher the score, the greater the possibility the individual will fall asleep during the daytime [11,14,25,27,30,33,34]. All women were classified according to ESS score. Those women who scored > 10 were included in the sleepy group and those women who scored ≤ 10 were included in the non-sleepy group [11,14,24,25,27,29,30,33-37].
Depression, anxiety, and stress were assessed using the Depression, Anxiety, and Stress Scale-21 (DASS-21). DASS-21 was a valid, reliable and a wide dimensional measure of psychological distress [38,39]. It has been widely used in studying perinatal psychological health [38-42]. Each item in DASS-21 was rated using a 4-point scale (0 for always false or not applicable to 3 for always true or totally applicable). DASS-21 is a validated tool in Ethiopia with the internal consistency reliability of Cronbach’s alpha of 0.75, 0.72, 0.86, and 0.95 for depression, anxiety, stress, and total scales, respectively [43]. Higher scores indicated greater distress levels. The cut-off values for DASS depression, anxiety and stress were 9, 7, and 14, respectively [38,41]. Based on the will of the women, those who had scores for Depression, Anxiety, and Stress Scales higher than the cut point were linked to the psychiatric ward for further diagnostic investigation.
Social support was assessed by the Oslo-3 social support scale, which is a 3-item questionnaire commonly used to assess social support with an internal consistency of α = 0.640 [44]. The scale asked about the ease of getting help from neighbors, the number of people the subjects can count on when there are serious problems, and the level of concern people show for what the subject was doing. A sum-index was obtained by adding the raw scores of the three items. The range was 3–14. The scores were interpreted as; 3–8 (poor social support), 9–11 (moderate social support), and 12–14 (strong social support) [45,46]. For screening of substance use, a modified form of Alcohol, Smoking, and Substance Involvement Screening Test (ASSIST), developed by the World Health Organization (WHO), an international group of substance abuse researchers, was used to detect and manage substance use and related problems in primary and general medical care settings.
Obstetric variables, such as pregnancy and labor complications, previous histories of stillbirth and previous history of abortion, planned current pregnancy, current pregnancy complications, and previous psychiatric histories, were collected by a structured and pre-tested questionnaire. A structured questionnaire was also used to collect information about the baby’s father’s support, the partner’s feelings about the current pregnancy, and substance use history.
Four Bachelor of Science graduating female clinical nurses and two Master of Science-graduating public health professionals were recruited as data collectors and supervisors, respectively. We modified the standard questionnaire for the evaluation of EDS and other parameters in order to attain data quality. A one-day training was given to both groups on the basic techniques of data collection procedures. One week before the actual data collection, a pretest was performed on 10% of the sample size in Haroye Health Post, and the data was not included in the final study. Daily supervision of the data collection process was implemented. The completeness and consistency of the collected data were checked daily by the supervisors and the principal investigator. The ethical approval of the study was received by the Institutional Review Board (IRB) of Wollo University College of Medicine and Health Science, Ethiopia (approval number: RCSPG-191/14). Ethical permission was obtained from Kutaber district Health office and Boru Meda Hospital. Before starting to fill out the questionnaire, written consent was obtained from every participant.
Statistical AnalysisData entry was performed using Epi-InfoTM version 7.1 (CDC, Atlanta, GA, USA). After full inspection of its completeness and consistency, it was then exported into Statistical Package for the Social Sciences SPSS window version 26 (IBM Corp., Armonk, NY, USA), for analysis. Categorical descriptive results were expressed using an actual number (frequency). To determine the association between independent and dependent variables, binary logistic regression was performed. Variables in bivariable analysis with a p < 0.2 were selected for multivariable logistic regression. In multivariable analysis, variables with a p < 0.05 with a 95% CI were considered significant factors of EDS. Hosmer and Lemshow goodness of fit tests were performed to assess model fitness at p > 0.05. Besides p-values, crude odds ratio and adjusted odds ratio (AOR) with 95% CI were reported.
RESULTSIn this study a total of 362 participants were included. The mean age of the participants was 30.4 ± 5.47 years. The minimum and maximum age of study subject were 18 and 45 years, respectively. Of these, 240 (66.3%) were found in 24–35 age group, 225 (62.2%) were rural residents. Most of the participants were Amhara in ethnicity (345, 95.3%), and were married (283, 78.2%), and 192 (53.0%) had housewife employment status (Table 1).
On pregnancy-related factors, 284 (78.5%) had a happy feeling of being pregnant; 267 (73.8%) reported that pregnancy was planned; 143 (39.5%) experienced excessive pregnancy-related feelings, 270 (74.6%) were delivered through normal vaginal delivery; and 171 (47.2%) had a history of obstetric complication.
Clinically, 147 (40.7%) people used substances in the past three months, 107 (29.6%) had a DASS-21 ≥ 10 of depression scale, and 90 (24.9%) had a chronic medical illness (Table 2).
Epworth Sleep Scale Scores of RespondentsThe lowest score of the data was 0 and the highest score was 19. The mean, median and mode the respondent was 6.8 ± 3.74, 7, 6, respectively. The scores above 10 were considered as the presence of excessive day time sleepiness (Fig. 1).
Accordingly, out of the 362 study subjects recruited for the study, 60 (16.6%) fulfilled the criteria for EDS as measured by the ESS. EDS (ESS score ≥ 11) was noted in 60 (16.6%) participants (Fig. 2).
Factors Associated with EDSAfter controlling for confounding effect of variables, excessive pregnancy related concern (AOR = 0.232, 95% CI: 0.087–0.621), having depression symptoms (AOR = 8.045, 95% CI: 3.375–19.174), anxiety symptoms (AOR = 4.905, 95% CI: 2.083–11.550) and having chronic medical illness (AOR = 5.441, 95% CI: 2.273–13.021) were the determinant factor of EDS (Table 3).
DISCUSSIONSleepiness affect performance in different ways. It is associated with sleepy episodes occurring during activities requiring a high degree of attention (driving a car) and may cause noticeable disruptions in social or occupational functioning [19]. Sleepiness also causing a broad range of neuropsychological deficits, including cognitive dysfunction, depression, and irritability [13,19,20,47]. Additionally, this degree of impairment in women during perinatal time may result in clear wakefulness, morbidity, accidents on herself and their child, and a variety of job and social situation limitations [48].
The aim of this study was to assess the prevalence of EDS and associated factors among women in the perinatal period at Kutaber Health Facility and Boru Meda General Hospital. The overall prevalence of EDS was 16.6% (95% CI: 12.6–20.7).
This result is in line with the other study conducted in Australia 13.6% [19] and 12.6% [49], in France 18.9 [50], in United Kingdom 18% [51], in Japan 14.9% [36] and 18.9% [29], in Korea 13.2% [17]. The finding in this study was higher when compared with the other study conducted in Switzerland 5.1% [31], in Japan 2.5% [52], in Slovakia 10.2% [30], in Sweden 7.9% [28], in China 10.9% [53]. In contrast, this result was less than the other study conducted in France 28% [18], in Korea 19.1% [47], in Brazil 55.5% [21], in France 35.3% [22], in Belgium 50.8% [33] and 34.3% [27], in China 22.2% [24], in Greece 38.8% [54] and in Nigeria 44.8% [55]. The discrepancy might be a result of a difference in assessment tools, geographical areas, sample size, the nature and culture of the study subject, and the study setting.
On the determinant factor, women with excessive pregnancy-related concern (AOR = 0.232, 95% CI: 0.087–0.621) experienced more daytime sleepiness than those who did not have excessive concern. This was due to excessive concern, which disturbs the internal function of the body system and leads to different complications like increased blood pressure, depression, anxiety, and others. Such type of complication especially depression leads daytime sleepiness.
The odds of having depression symptoms in perinatal time (AOR = 8.045, 95% CI: 3.375–19.174) were 8 times higher than those who have not depression symptoms. The result was analogous to other studies conducted in France [18], Brazil [21], two different studies in Australia [19,49], and New Zealand [56], and in Korea [47]. This might be because higher levels of cortisol, corticotropic releasing hormone, and norepinephrine during depression lead to sleep rhythm disruption that ends up with EDS [55]. Sleeping too much could be a symptom of depression.
Parallel to many other studies conducted elsewhere [15,52], the odds of having anxiety symptoms (AOR = 4.905, 95% CI: 2.083–11.550) were four times higher than those who did not show anxiety symptoms. These may be due to long-term exposure to anxiety, which causes the hypothalamus, pituitary, and adrenal glands to release hormones to prepare for fight, flee, or freeze. In response they experienced a feeling of exhaustion, were physically fatigued, and may have difficulty falling asleep or staying asleep at night. Otherwise, they may oversleep during the day.
The odds of having chronic medical illness (AOR = 5.441, 95% CI: 2.273–13.021) were five times greater than for those women without chronic medical illness. This was consistent with other study in France [50] and [18], Canada [16], Australia [19] and Slovakia [30]. The possible clarification is the pain and fatigue of chronic medical illness have impact on women daily activities including sleep quality [16,19,50]. Because of their illness they often experience sleeping problems at night and they become sleepy during day time. Indirectly, the illness also leads other health problems like depression and/or anxiety, which can also cause EDS.
Other study also reported that the association of EDS to younger age [20,52] male sex [49,52], smoking [18], high degree of job [22], insomnia [13,18], loud snoring [16,20,52], and multiple gestations [20]. Though, all the above factors were not independent predictors of EDS in our study, this might be due to variations in sample size, life style, health status, and sociocultural factors of the study subjects. The findings of this study suggested that women in perinatal period are susceptible to EDS that is associated with depression, anxiety and medical illness. If not appropriately handled, EDS could lead to poor quality of maternal and child health [48]. Objective measures of sleepiness were not available for this study. So, the study has some limitations. Selection bias may exist even if systematic random selection was used for the recruitment of the participants. The responses the questionnaire may depend on the participant’s perceptual experience as a result recall bias occurred.
In conclusion, perinatal EDS is high and significantly associated with excessive pregnancy-related concern, depression, anxiety, and chronic medical illness. This suggested the need to encourage women to get counseling on how to cope with the pregnancy-related biological, physical, social, and emotional changes in the environment, which is important to reduce the associated factor. Health institutions should establish guidance and counseling services when the women get them during perinatal care. Furthermore, we recommend future researchers undertake studies using strong designs and qualitative studies to find out the factors affecting EDS.
NOTESAvailability of Data and Material
The datasets generated or analyzed during the study are available from the corresponding author on reasonable request.
Authors’ Contribution
Conceptualization: Jemal Seid, Emam Mohammed. Data curation: Jemal Seid. Formal analysis: Jemal Seid. Funding acquisition: Emam Mohammed. Methodology: all authors. Project administration: Jemal Seid, Emam Mohammed, Hassen Yimer Hassen. Resources: Jemal Seid, Emam Mohammed. Software: Jemal Seid, Emam Mohammed. Supervision: Jemal Seid, Emam Mohammed, Hassen Yimer Hassen. Validation: Jemal Seid, Bilal Mohammed Aman, Hassen Yimer Hassen. Visualization: all authors. Writing—original draft: Jemal Seid. Writing—review & editing: all authors.
ACKNOWLEDGEMENTSThe authors would like to acknowledge the staff of Wollo University, study participants, and data collectors for their welcome and assistance and also to Kutaber district administrative office for allowing funds to conduct this study. Finally, our special gratitude goes to all peoples who formally or informally gave us support to accomplish this study.
REFERENCES1. Sousa VPSD, Ribeiro SO, Aquino CMRD, Viana EDSR. Quality of sleep in pregnant woman with low back pain. Fisioter Mov 2015;28:319-26.
2. Creti L, Libman E, Rizzo D, Fichten CS, Bailes S, Tran DL, et al. Sleep in the postpartum: characteristics of first-time, healthy mothers. Sleep Disord 2017;2017:8520358.
3. Moghadam ZB, Rezaei E, Rahmani A. Sleep disorders during pregnancy and postpartum: a systematic review. Sleep Med Res 2021;12:81-93.
4. Zhang D, Zhang Z, Li H, Ding K. Excessive daytime sleepiness in depression and obstructive sleep apnea: more than just an overlapping symptom. Front Psychiatry 2021;12:710435.
5. Bourjeily G, El Sabbagh R, Sawan P, Raker C, Wang C, Hott B, et al. Epworth sleepiness scale scores and adverse pregnancy outcomes. Sleep Breath 2013;17:1179-86.
6. Smyka M, Kosińska-Kaczyńska K, Sochacki-Wójcicka N, Zgliczyńska M, Wielgoś M. Sleep problems in pregnancy-a cross-sectional study in over 7000 pregnant women in Poland. Int J Environ Res Public Health 2020;17:5306.
7. Fernández-Alonso AM, Trabalón-Pastor M, Chedraui P, Pérez-López FR. Factors related to insomnia and sleepiness in the late third trimester of pregnancy. Arch Gynecol Obstet 2012;286:55-61.
8. Salari N, Darvishi N, Khaledi-Paveh B, Vaisi-Raygani A, Jalali R, Daneshkhah A, et al. A systematic review and meta-analysis of prevalence of insomnia in the third trimester of pregnancy. BMC Pregnancy Childbirth 2021;21:284.
9. Cai XH, Xie YP, Li XC, Qu WL, Li T, Wang HX, et al. The prevalence and associated risk factors of sleep disorder-related symptoms in pregnant women in China. Sleep Breath 2013;17:951-6.
10. Kalmbach DA, Cheng P, Roth A, Roth T, Swanson LM, O’Brien LM, et al. DSM-5 insomnia disorder in pregnancy: associations with depression, suicidal ideation, and cognitive and somatic arousal, and identifying clinical cutoffs for detection. Sleep Adv 2022;3:zpac006.
11. Lee HJ, Oh KS, Kim T, Lee CS, Jeong J, Youn SY, et al. Prevalence, risk factors, and impact of excessive daytime sleepiness in an elderly Korean population. Sleep Med Res 2014;5:54-61.
12. Etindele-Sosso FA. Insomnia, excessive daytime sleepiness, anxiety, depression and socioeconomic status among customer service employees in Canada. Sleep Sci 2020;13:54-64.
13. Dagnew B, Andualem Z, Dagne H. Excessive daytime sleepiness and its predictors among medical and health science students of University of Gondar, Northwest Ethiopia: institution-based cross-sectional study. Health Qual Life Outcomes 2020;18:299.
14. Hunskar GS, Bjorvatn B, Wensaas KA, Hanevik K, Eide GE, Langeland N, et al. Excessive daytime sleepiness, sleep need and insomnia 3 years after Giardia infection: a cohort study. Sleep Health 2016;2:154-8.
15. Mindell JA, Cook RA, Nikolovski J. Sleep patterns and sleep disturbances across pregnancy. Sleep Med 2015;16:483-8.
16. van der Spuy I, Karunanayake CP, Dosman JA, McMullin K, Zhao G, Abonyi S, et al. Determinants of excessive daytime sleepiness in two First Nation communities. BMC Pulm Med 2017;17:192.
17. Kim SM, Um YH, Kim TW, Jeong JH, Seo HJ, Song JH, et al. Excessive daytime sleepiness and its risk factors for commercial bus drivers in Korea. Sleep Med Res 2017;8:76-80.
18. Jaussent I, Morin CM, Ivers H, Dauvilliers Y. Incidence, worsening and risk factors of daytime sleepiness in a population-based 5-year longitudinal study. Sci Rep 2017;7:1372.
19. Hayley AC, Williams LJ, Kennedy GA, Holloway KL, Berk M, Brennan-Olsen SL, et al. Excessive daytime sleepiness and falls among older men and women: cross-sectional examination of a population-based sample. BMC Geriatr 2015;15:74.
20. Bourjeily G, Raker C, Chalhoub M, Miller M. Excessive daytime sleepiness in late pregnancy may not always be normal: results from a cross-sectional study. Sleep Breath 2013;17:735-40.
21. Medeiros C, Bruin V, Férrer D, Paiva T, Montenegro Júnior R, Forti A, et al. Excessive daytime sleepiness in type 2 diabetes. Arq Bras Endocrinol Metabol 2013;57:425-30.
22. Sabil A, Bignard R, Gervès-Pinquié C, Philip P, Le Vaillant M, Trzepizur W, et al. Risk factors for sleepiness at the wheel and sleep-related car accidents among patients with obstructive sleep apnea: data from the French pays de la Loire sleep cohort. Nat Sci Sleep 2021;13:1737-46.
23. Hein M, Lanquart JP, Loas G, Hubain P, Linkowski P. Prevalence and risk factors of excessive daytime sleepiness in insomnia sufferers: a study with 1311 individuals. J Psychosom Res 2017;103:63-9.
24. Wu S, Wang R, Ma X, Zhao Y, Yan X, He J. Excessive daytime sleepiness assessed by the Epworth sleepiness scale and its association with health related quality of life: a population-based study in China. BMC Public Health 2012;12:849.
25. Signal TL, Paine SJ, Sweeney B, Priston M, Muller D, Smith A, et al. Prevalence of abnormal sleep duration and excessive daytime sleepiness in pregnancy and the role of socio-demographic factors: comparing pregnant women with women in the general population. Sleep Med 2014;15:1477-83.
26. Jacobsen JH, Shi L, Mokhlesi B. Factors associated with excessive daytime sleepiness in patients with severe obstructive sleep apnea. Sleep Breath 2013;17:629-35.
27. Boz S, Lanquart JP, Mungo A, Delhaye M, Loas G, Hein M. Risk of excessive daytime sleepiness associated to major depression in adolescents. Psychiatr Q 2021;92:1473-88.
28. Theorell-Haglöw J, Åkerstedt T, Schwarz J, Lindberg E. Predictors for development of excessive daytime sleepiness in women: a population-based 10-year follow-up. Sleep 2015;38:1995-2003.
29. Ohashi M, Kohno T, Kohsaka S, Fukuoka R, Hayashida K, Yuasa S, et al. Excessive daytime sleepiness is associated with depression scores, but not with sleep-disordered breathing in patients with cardiovascular diseases. Circ J 2018;82:2175-83.
30. Šiarnik P, Klobučníková K, Šurda P, Putala M, Šutovský S, Kollár B, et al. Excessive daytime sleepiness in acute ischemic stroke: association with restless legs syndrome, diabetes mellitus, obesity, and sleep-disordered breathing. J Clin Sleep Med 2018;14:95-100.
31. Berger M, Hirotsu C, Haba-Rubio J, Betta M, Bernardi G, Siclari F, et al. Risk factors of excessive daytime sleepiness in a prospective population-based cohort. J Sleep Res 2021;30:e13069.
32. Manzar MD, Salahuddin M, Alamri M, Albougami A, Khan MYA, Nureye D, et al. Psychometric properties of the Epworth sleepiness scale in Ethiopian university students. Health Qual Life Outcomes 2019;17:30.
33. Hein M, Lanquart JP, Loas G, Hubain P, Linkowski P. Prevalence and risk factors of excessive daytime sleepiness in major depression: a study with 703 individuals referred for polysomnography. J Affect Disord 2019;243:23-32.
34. Prasad B, Steffen AD, Van Dongen HPA, Pack FM, Strakovsky I, Staley B, et al. Determinants of sleepiness in obstructive sleep apnea. Sleep 2018;41:zsx199.
35. Zhang F, Wu X, Duan W, Wang F, Huang T, Xiang M. Influencing factors of daytime sleepiness in patients with obstructive sleep apnea hypopnea syndrome and its correlation with pulse oxygen decline rate. Evid Based Complement Alternat Med 2021;2021:6345734.
36. Kawada T. Excessive daytime sleepiness, depression and sleep-disordered breathing in patients with cardiovascular disease. Circ J 2019;83:692.
37. Ronksley PE, Hemmelgarn BR, Heitman SJ, Flemons WW, Ghali WA, Manns B, et al. Excessive daytime sleepiness is associated with increased health care utilization among patients referred for assessment of OSA. Sleep 2011;34:363-70.
38. Tran TD, Tran T, Fisher J. Validation of the depression anxiety stress scales (DASS) 21 as a screening instrument for depression and anxiety in a rural community-based cohort of northern Vietnamese women. BMC Psychiatry 2013;13:24.
39. Rusli BN, Amrina K, Trived S, Loh KP, Shashi M. Construct validity and internal consistency reliability of the Malay version of the 21-item depression anxiety stress scale (Malay-DASS-21) among male outpatient clinic attendees in Johor. Med J Malaysia 2017;72:264-70.
40. Lydon K, Dunne FP, Owens L, Avalos G, Sarma KM, O’Connor C, et al. Psychological stress associated with diabetes during pregnancy: a pilot study. Ir Med J 2012;105(5 Suppl):26-8.
41. Basha E, Kaya M. Depression, anxiety and stress scale (DASS): the study of validity and reliability. Univers J Educ Res 2016;4:2701-5.
42. Pezirkianidis C, Karakasidou E, Lakioti A, Stalikas A, Galanakis M. Psychometric properties of the depression, anxiety, stress scales-21 (DASS-21) in a Greek sample. Psychology 2018;9:2933-50.
43. Damota MD, Robe E. Depression, anxiety and stress among first year addis Ababa university students: magnitude, and relationship with academic achievement. J Health Med Nurs 2018;56:53-9.
44. Kocalevent RD, Berg L, Beutel ME, Hinz A, Zenger M, Härter M, et al. Social support in the general population: standardization of the Oslo social support scale (OSSS-3). BMC Psychol 2018;6:31.
45. Jemal K. Prevalence and correlates of co-morbid anxiety and depression among patients with dental disease on follow up at Saint Paul’s hospital millennium medical college, Addis Ababa, Ethiopia. J Am Sci 2018;14:77-83.
46. Ibrahim AW, Mukhtar Y, Sadique P, Tahir BM, Olabisi AM, Bukar RI, et al. A facility-based assessment of internalized stigma among patients with severe mental illnesses in Maiduguri, North-Eastern Nigeria. Int Neuropsychiatr Dis J 2016;6:1-11.
47. Sunwoo JS, Shin DS, Hwangbo Y, Kim WJ, Chu MK, Yun CH, et al. High risk of obstructive sleep apnea, insomnia, and daytime sleepiness among commercial motor vehicle drivers. Sleep Breath 2019;23:979-85.
48. Sawan P, El Sabbagh R, Raker C, Bourjeily G. Does excessive daytime sleepiness contribute to worse outcomes in pregnancy? Chest 2011;140:448A.
49. Adams RJ, Appleton SL, Vakulin A, Lang C, Martin SA, Taylor AW, et al. Association of daytime sleepiness with obstructive sleep apnoea and comorbidities varies by sleepiness definition in a population cohort of men. Respirology 2016;21:1314-21.
50. Empana JP, Dauvilliers Y, Dartigues JF, Ritchie K, Gariepy J, Jouven X, et al. Excessive daytime sleepiness is an independent risk indicator for cardiovascular mortality in community-dwelling elderly: the three city study. Stroke 2009;40:1219-24.
51. Slater G, Steier J. Excessive daytime sleepiness in sleep disorders. J Thorac Dis 2012;4:608-16.
52. Kaneita Y, Ohida T, Uchiyama M, Takemura S, Kawahara K, Yokoyama E, et al. Excessive daytime sleepiness among the Japanese general population. J Epidemiol 2005;15:1-8.
53. Li X, Huang H, Xu H, Shi Y, Qian Y, Zou J, et al. Excessive daytime sleepiness, metabolic syndrome, and obstructive sleep apnea: two independent large cross-sectional studies and one interventional study. Respir Res 2019;20:276.
Fig. 1.The frequency of the Epworth Daytime Sleepiness Scale (ESS) response among women in perinatal period (n = 362). 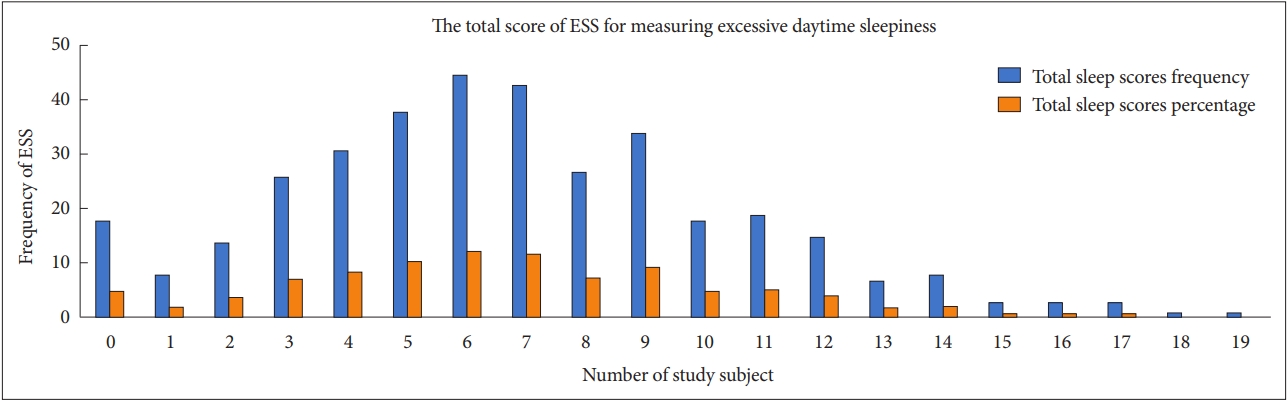
Fig. 2.The prevalence of excessive daytime sleepiness (EDS) among women in perinatal period (n = 362). 
Table 1.Sociodemographic characteristics of study subjects (n = 362) Table 2.Pregnancy and clinical characteristic of study subject (n = 362) Table 3.Factors associated with excessive daytime sleepiness in perinatal period (n = 362)
|
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||