AbstractBackground and ObjectiveWe explored in this study whether insomnia, viral anxiety, reassurance-seeking behavior, and preoccupation with coronavirus disease (COVID-19) are related among the general population. As well, we explored the possibility that insomnia may mediate the association between COVID-19 viral anxiety and preoccupation.
MethodsDuring November 9–15, 2021, 400 participants voluntarily completed this survey, and participants’ age, sex, living location, and marital status were collected. Responses to questions about COVID-19 were also gathered, and their symptoms were rated using the Obsession with COVID-19 Scale (OCS), Coronavirus Reassurance-Seeking Behaviors Scale (CRBS), Fear of COVID-19 scale (FCV-19S), and Insomnia Severity Index (ISI).
ResultsPreoccupation with COVID-19 was predicted by young age (β = -0.08, p = 0.012), CRBS (β = 0.52, p < 0.001), FCV-19S (β = 0.30, p < 0.001), and ISI (β = 0.07, p = 0.029) (adjusted R2 = 0.62, F = 163.6, p < 0.001). Mediation analysis showed that insomnia partially mediates the influence of reassurance seeking behavior and viral anxiety on preoccupation with COVID-19.
INTRODUCTIONThe coronavirus disease (COVID-19) pandemic has brought about many changes, and psychological distress is one of them. There has been a survey study in China to investigate the association between mental health symptoms, including depression and anxiety, and their prevalence and risk factors during the COVID-19 pandemic. In this study, depressive symptoms were reported in 27.9% and anxiety symptoms in 31.6%, and those with confirmed or suspected COVID-19, those at risk of occupational exposure, and residents of Hubei Province had more severe symptoms [1]. In Spain, as a result of surveying the degree of depression and anxiety among the general population during the COVID-19 pandemic through an online survey, 27.5% of participants reported severe depression and 20.8% of severe anxiety [2].
Coronavirus-Related Reassurance Seeking and Preoccupation with COVID-19High prevalence of psychiatric disorders in pandemics has been reported in several studies. A study of severe acute respiratory syndrome (SARS) is about significant rates of psychiatric morbidity related to SARS [3]. Approximately 75% of participants changed their behavior because of fear of infection, and some of them also showed emotional distress in the H1N1 epidemic [4]. People not diagnosed with Middle East respiratory syndrome (MERS), but isolated, experienced anxiety in 7.6% of cases and anger in 16.6% of cases [5]. Even in the COVID-19 pandemic, these psychiatric-related problems were observed. According to a study with more than 2000 participants during the COVID-19 pandemic, anxiety is prevalent in about 34% of the population [6]. Systematic review and meta-analysis studies of COVID-19 pandemic populations revealed that anxiety and depression are common among more than 30% of those affected [7]. Also, COVID-19 is associated with depression severity in the general population [8].
Fear of contamination and excessive checking are the symptoms most frequently associated with COVID-19 [9-11]. Additionally, those who wear masks and wash their hands are significantly more likely to fear contamination, as their characteristics correlate with behaviors that reduce the spread of infection. The model of hypochondriasis (currently known as Illness Anxiety Disorder) states that fear of being sick leads to anxiety, which leads one to avoid the problem or seek reassurance [12]. An illness anxiety cognitive-behavioral model suggests that when someone is anxious about getting ill, they try to avoid the problem or seek reassurance. Getting immediate relief from reassurance strengthened one’s original fear, which will contribute to preoccupation with the illness. It will cause preoccupation with the illness if this process continues.
In this COVID-19 pandemic, if one is afraid of being infected in this COVID-19 pandemic, then one may engage in reassurance-seeking behavior, such as checking bodily sensation, maintaining hand hygiene, or reading repeated media articles [13]. Recurrently engaging in reassurance-seeking behaviors may paradoxically increase anxiety. When people are worried about their health or feel anxious about it in some way, they seek reassurance, which can be a sign of preoccupation with COVID-19 viral infection. We all experience some degree of health anxiety at some point in our lives, and these behaviors can help us identify and protect against illnesses in the early stages. Recurrent engagement in reassurance-seeking behaviors, however, increases anxiety [14]. Excessive consumption of media and distress are often related to anxiety and uncertainty, creating a cycle that is difficult to break. People with high health anxiety must constantly seek reassurance, which can result in them resorting to reassurance-seeking behavior [15].
Insomnia and Vial Anxiety in COVID-19A number of studies were conducted which explored the relationship between viral anxiety, feelings provoked by worries about exposure to virus and infection and insomnia during the COVID-19 pandemic. It is well known that insomnia symptoms were associated with depression or anxiety [7]. In COVID-19 pandemic, a study found that viral anxiety was a consistent predictor of insomnia [16]. Stress, anxiety, and depression may be more likely to occur in individuals suffering from pre-existing and post-pandemic insomnia during the COVID-19 pandemic [17]. And, those who are uncertain as to whether they will contract COVID-19 and fear direct contact with COVID-19 infected individuals are at greater risk for sleep disturbances [18]. University students who fear catching COVID-19 significantly experienced higher levels of anxiety or insomnia [19], and dysfunctional beliefs about sleep of cancer patients mediated the effects of anxiety on functional impairment [20]. Among healthcare workers, insomnia mediates the effects of viral epidemics on anxiety and depression [21]. However, it has not yet been studied empirically on the relationship between insomnia and coronavirus reassurance-seeking behavior, though it has been reported that obsessive compulsive symptoms may increase in those with insomnia symptoms before the coronavirus pandemic [22]. Because of the connection between sleep disorders and anxiety, as well as high-risk factors that make humans particularly susceptible to viral infections during this pandemic [23], it is important to understand the mediating effect of insomnia on the enhancement mechanism of anxiety symptoms.
In this study we aimed to explore whether insomnia, viral anxiety, reassurance-seeking behavior, and preoccupation with COVID-19 are related among the general population in this study. In addition, we tried to explore whether insomnia may mediate the viral anxiety and preoccupation with COVID-19. We hypothesized that 1) reassurance-seeking behavior will be positively related to preoccupation with COVID-19, 2) viral anxiety will be positively associated with preoccupation with COVID-19, 3) insomnia will be positively associated with preoccupation with COVID-19, and 4) insomnia will at least partially mediate the relationships between reassurance-seeking behavior and preoccupation with COVID-19 among the general population.
METHODSSurveys were conducted anonymously during November 9–15, 2021, and 400 participants voluntarily participated in this study after checking “yes” to the statement of agreeing to participate. They completed it through the survey system of professional survey company EMBRAIN (www.embrain.com). Participants’ age, sex, living location, and marital status were collected, but no personally identifiable information was collected. We also gathered responses to questions about COVID-19, such as “Did you experience being quarantined due to infection with COVID-19?”, “Did you experience being infected with COVID-19?”, or “Did you get vaccinated?” Additionally, participants’ past psychiatric history was checked with a question such as “Have you ever suffered depression, anxiety, or insomnia?” and current psychiatric distress with a question of “Now, do you think you are depressed or anxious, or do you need help for your mood state?” Before the investigators received the data, all identifying personal information was removed. Asan Medical Center’s Institutional Review Board (IRB) approved the study protocol (2021-1490), and the IRB waived obtaining written informed consent.
AssessmentObsession with COVID-19 ScaleThe Obsession with COVID-19 Scale (OCS) is a self-report mental health screening tool that measures persistently disturbing thoughts related to COVID-19 [24]. Moreover, it can help identify individuals who have thinking patterns that are associated with COVID-19 that are functionally impaired. The OCS has four items, each of which is rated on a 5-point scale from 0 (not at all) to 4 (nearly every day over the last two weeks). Scores ≥ 7 indicate likely dysfunctional thinking about COVID-19. In this study, we applied Korean version of OCS [25] and Cronbach’s alpha in this sample was 0.854.
Coronavirus Reassurance-Seeking Behaviors ScaleCoronavirus Reassurance-Seeking Behaviors Scale (CRBS) is a self-report measure of reassurance-seeking behaviors associated with concerns about Coronavirus infection [26]. To be on the lookout for signs and symptoms of COVID-19 infection is advisable. Excessive behavior seeking reassurance, however, may cause anxiety in some people. CRBS was designed to measure excessive reassurance seeking behavior of people seeking information related to Coronaviruses. Five items are rated from 0 (not at all) to 4 (nearly every day). In this study, we applied the Korean version of the CRBS [27], and Cronbach’s alpha in this sample was 0.867.
Fear of COVID-19 scaleA self-rating questionnaire, Fear of COVID-19 scale (FCV-19S), can be used to measure viral anxiety during a COVID-19 pandemic [28]. The questionnaire includes seven items, each of which can be rated on a 5-point Likert scale from 1 (strongly disagree) to 5 (strongly agree). High total score is indicative of a more severe level of viral anxiety. We applied the Korean version of the FCV-19S [29], and Cronbach’s alpha was 0.927 in this sample.
Insomnia Severity IndexAn Insomnia Severity Index (ISI) is designed to measure insomnia severity [30]. There are seven items to be scored on a 5-point Likert scale, yielding a score ranging from 0 to 28. A higher total score reflects a severe insomnia. In this study, we applied Korean version of the ISI [31], and Cronbach’s alpha among this sample was 0.858.
Statistical AnalysisThe mean and standard deviation of participants’ demographic characteristics and rating scale scores are summarized. Two-tailed significance was determined by a p value of 0.05. Correlation analysis was performed using Pearson’s correlation coefficient. We used linear regression to examine which variables can predict obsession with COVID-19. The bootstrap method with 2000 resamples was implemented to determine whether insomnia mediates the influence of viral anxiety or reassurance seeking behavior on preoccupation with COVID-19. The SPSS version 21.0 (IBM Co., Armonk, NY, USA) was used to conduct the general statistical analysis, and AMOS version 27 (IBM Co.) and Jamovi ver 1.6.23 (The jamovi project, Sydney, NSW, Australia) were used to conduct the mediation analysis.
RESULTSAmong the 400 participants were residents of Seoul (n = 117, 29.3%), Pusan (n = 30, 7.5%), Daegu (n = 18, 4.5%), Daejeon (n = 9, 2.3%), Gwangju (n = 10, 2.5%), Incheon (n = 31, 7.8%), Ulsan (n = 8, 2.0%), Gyeonggi Province (n = 108, 27.0%), Chungcheong Province (n = 20, 5.0%), Jeolla Province (n = 11, 2.8%), Gyeongsang Province (n = 29, 7.3%), Gangwon Province (n = 7, 1.8%), and Jeju Province (n = 2, 0.5%). Demographic characteristics of participants were presented in Table 1.
Pearson’s correlation analysis showed that age was significantly correlated with OCS (r = -0.23, p < 0.01), CRBS (r = -0.26, p < 0.01), and ISI (r = -0.17, p < 0.01). The OCS score was significantly correlated with CRBS (r = 0.74, p < 0.01), FCV-19S (r = 0.63, p < 0.01), and ISI (r = 0.37, p < 0.01). The CRBS was significantly correlated with FCV-19S (r = 0.59, p < 0.01) and ISI (r = 0.34, p < 0.01). FCV-19S was correlated with ISI (r = 0.36, p < 0.01) (Table 2).
Linear regression analysis was done to explore which variables can predict the preoccupation with COVID-19, and we observed that preoccupation with COVID-19 was expected by age (β = -0.08, p = 0.012), CRBS (β = 0.52, p < 0.001), FCV-19S (β = 0.30, p < 0.001), and ISI (β = 0.07, p = 0.029) (adjusted R2 = 0.62, F = 163.6, p < 0.001) (Table 3).
Mediation analysis showed that the complete pathway from reassurance-seeking behavior or viral anxiety (independent variable) to insomnia (mediator) to preoccupation with COVID-19 (dependent variable) was significant (Table 4) indicating that insomnia partially mediates the influence of reassurance seeking behavior and viral anxiety on preoccupation with COVID-19 (Fig. 1).
DISCUSSIONIn this study, we investigated whether insomnia, viral anxiety, reassurance seeking behavior, and preoccupation with COVID-19 are related among the general population. Moreover, we investigated whether insomnia may mediate COVID-19 anxiety and preoccupation. We observed that preoccupation with COVID-19 was predicted by younger age, coronavirus reassurance seeking, and viral anxiety or insomnia severity. Additionally, we observed that insomnia partially mediated the influence of reassurance seeking behavior and viral anxiety on preoccupation with COVID-19.
Preoccupation with COVID-19, Viral Anxiety, and Reassurance-Seeking BehaviorPreoccupation with COVID-19 virus was associated with younger age, insomnia, viral anxiety, and reassurance-seeking behavior in this study. Vicious cycle among viral anxiety, reassurance-seeking, and preoccupation with COVID-19 was already reported. We reported previously that the reassurance seeking behavior of healthcare workers and their preoccupation with COVID-19 were associated with work-related stress and viral anxiety of healthcare workers [32]. In addition, among medical students, preoccupation with COVID-19 was reported to be predicted by viral anxiety and reassurance-seeking behavior [32], similarly to the results of the current study. Having anxiety about viral infection is beneficial to protect from infection, but excessive anxiety and obsessive thinking can be detrimental to mental health. Since this COVID-19 pandemic has lasted for a long time, persistent anxiety and obsessional thoughts should be managed. When people feel anxious, they may seek assurance to reduce their anxiety and risk of harm. Therefore, they may engage in reassurance-seeking behaviors such as checking their body temperature, repeating hand washing, or monitoring their physical symptoms. In the short-term, reassurance-seeking behavior may reduce anxiety briefly, but in the long run, it may strengthen the tendency to seek reassurance. Although it is not always easy to distinguish repeated handwashing as a reassurance-seeking behavior from a preventive measure, hypochondriacal fears may trigger reassurance-seeking behaviors [33]. In addition, cyberchondria, which is an excessive online health search associated with higher levels of anxiety and reassurance-seeking behavior, is made worse by repetitive, misleading information that is spread on social media.
Age and preoccupation with COVID-19 are inversely correlated, and this relationship is complicated. Having an underlying medical condition and old age were risk factors for COVID-19 infection [34]. As a result, the older are likely to be aware of their vulnerability to infection. The result may be a stabilized cautious lifestyle regardless of other informative influences. In contrast, young people can easily access the information of COVID-19 via the internet, and they are more likely to seek reassurance repeatedly. These points need to be explored in the further study.
Insomnia as a Mediator of the Vicious Cycle of Hypochondriacal Preoccupation with COVID-19In this study, we observed that reassurance-seeking behavior and viral anxiety were predicting variables for preoccupation with COVID-19. And also, we observed that insomnia can be a mediator on this vicious cycle model of hypochondriacal preoccupation. In this COVID-19, high prevalence of insomnia was reported. Approximately 38% of participants in Greek population-based study reported that sleep problems [35]. Other two studies covering general population associated with COVID-19 also showed that higher prevalence of sleep disturbance each about 19% and 13% of participants [36,37]. Sleep disturbances are known to be associated with the weakened immune system, and a weakened immune system increases the risk of viral infection [38]. If they cannot sleep well, people may worry about getting infected with a virus as a dysfunctional belief about sleep. Consequently, insomnia can increase an individual’s anxiety levels [39]. In other words, insomnia exacerbates anxiety and concerns about viral infections. As a consequence, there is an increase in reassurance seeking behaviors like fever checking, symptom evaluation, and internet browsing, and as insomnia persists, reassurance seeking behaviors increase, and people become obsessed with COVID-19 information. Our study provides significant insight by revealing that insomnia mediates this process.
This study has some limitations. First, the online survey design has the potential to cause bias. In order to prevent the spread of the virus during this pandemic era, we decided to conduct an online survey rather than a face-to-face interview. However, the responses may not be as reliable as they seem. Second, the result of a small sample size cannot be applied to the entire population. The sample we collected included similar allocation by sex, age group, and entire area of Korea, and we could improve the representativeness of the sample. Third, Since COVID-19, viral anxiety, reassurance seeking, and insomnia are related to anxiety, there needs to be caution when explaining their connection. Moreover, there could be confounders not considered in this study, such as occupation, education level, or social economic status, that might affect the results. Lastly, the study took place from November 9–15, 2021. The Korean government started implementing the “living with Coronavirus” policy starting November 1st, 2021, and soon the number of confirmed cases exceeded 7000 per day. Although the rapid spread of the virus may affect these results, we should also take into account the fact at the same time that people have already become used to 2 years of pandemic.
In conclusion, we observed that insomnia partially mediated the vicious cycle of the hypochondriacal preoccupation with COVID-19 linked to reassurance seeking-behavior and viral anxiety. Sleep specialists should address the insomnia symptoms of people in order to reduce viral anxiety and repetitive reassurance-seeking behavior that can contribute to the preoccupation with COVID-19.
NOTESAvailability of Data and Material
The datasets generated or analyzed during the study are available from the corresponding author on reasonable request.
Authors’ Contributions
Conceptualization: Young Rong Bang, Junseok Ahn. Data curation: Eulah Cho, Inn-Kyu Cho, Dongin Lee, Joohee Lee. Formal analysis: Eulah Cho, Inn-Kyu Cho, Dongin Lee, Joohee Lee. Methodology: Young Rong Bang, Eulah Cho. Visualization: Dongin Lee, Joohee Lee. Writing—original draft: all authors. Writing—review & editing: all authors.
ACKNOWLEDGEMENTSWe would like to thank Dr. Seockhoon Chung (Department of Psychiatry, University of Ulsan College of Medicine) for the ideas of and wonderful discussion about this study.
REFERENCES1. Li D, Zou L, Zhang Z, Zhang P, Zhang J, Fu W, et al. The psychological effect of COVID-19 on home-quarantined nursing students in China. Front Psychiatry 2021;12:652296.
2. Galindo-Vázquez O, Ramírez-Orozco M, Costas-Muñiz R, Mendoza-Contreras LA, Calderillo-Ruíz G, Meneses-García A. Symptoms of anxiety, depression and self-care behaviors during the COVID-19 pandemic in the general population. Gac Med Mex 2020;156:298-305.
3. Sim K, Chan YH, Chong PN, Chua HC, Soon SW. Psychosocial and coping responses within the community health care setting towards a national outbreak of an infectious disease. J Psychosom Res 2010;68:195-202.
4. Lau JT, Griffiths S, Choi KC, Tsui HY. Avoidance behaviors and negative psychological responses in the general population in the initial stage of the H1N1 pandemic in Hong Kong. BMC Infect Dis 2010;10:139.
5. Jeong H, Yim HW, Song YJ, Ki M, Min JA, Cho J, et al. Mental health status of people isolated due to Middle East Respiratory Syndrome. Epidemiol Health 2016;38:e2016048.
6. Necho M, Tsehay M, Birkie M, Biset G, Tadesse E. Prevalence of anxiety, depression, and psychological distress among the general population during the COVID-19 pandemic: a systematic review and meta-analysis. Int J Soc Psychiatry 2021;67:892-906.
7. Wang Y, Kala MP, Jafar TH. Factors associated with psychological distress during the coronavirus disease 2019 (COVID-19) pandemic on the predominantly general population: a systematic review and meta-analysis. PLoS One 2020;15:e0244630.
9. Dennis D, Radnitz C, Wheaton MG. A perfect storm? Health anxiety, contamination fears, and COVID-19: lessons learned from past pandemics and current challenges. Int J Cogn Ther 2021;14:497-513.
10. Knowles KA, Olatunji BO. Anxiety and safety behavior usage during the COVID-19 pandemic: the prospective role of contamination fear. J Anxiety Disord 2021;77:102323.
11. Ojalehto HJ, Abramowitz JS, Hellberg SN, Butcher MW, Buchholz JL. Predicting COVID-19-related anxiety: the role of obsessive-compulsive symptom dimensions, anxiety sensitivity, and body vigilance. J Anxiety Disord 2021;83:102460.
12. Mousavi SM, Yazdanirad S, Sadeghian M, Abbasi M, Jahadi Naeini M. Relationship between resilience and hypochondriasis due to COVID-19: a case study in an occupational environment. J Occup Hyg Eng 2021;7:35-43.
13. Lee SA, Crunk EA. Fear and psychopathology during the COVID-19 crisis: neuroticism, hypochondriasis, reassurance-seeking, and coronaphobia as fear factors. Omega (Westport) 2022;85:483-96.
14. Carleton RN, Desgagné G, Krakauer R, Hong RY. Increasing intolerance of uncertainty over time: the potential influence of increasing connectivity. Cogn Behav Ther 2019;48:121-36.
15. Hoory L. The psychology of reassurance seeking — and why it can be toxic for people with OCD. [cited 2022 May 23]. Available from: https://www.treatmyocd.com/blog/reassurance-seeking-ocd-anxiety-how-to-stop-cycle.
16. Brown LA, Hamlett GE, Zhu Y, Wiley JF, Moore TM, DiDomenico GE, et al. Worry about COVID-19 as a predictor of future insomnia. J Sleep Res 2022 Feb 14;[Epub]. https://doi.org/10.1111/jsr.13564.
17. Meaklim H, Junge MF, Varma P, Finck WA, Jackson ML. Pre-existing and post-pandemic insomnia symptoms are associated with high levels of stress, anxiety, and depression globally during the COVID-19 pandemic. J Clin Sleep Med 2021;17:2085-97.
18. Casagrande M, Favieri F, Tambelli R, Forte G. The enemy who sealed the world: effects quarantine due to the COVID-19 on sleep quality, anxiety, and psychological distress in the Italian population. Sleep Med 2020;75:12-20.
19. Vilca LW, Chávez BV, Fernández YS, Caycho-Rodríguez T, White M. Impact of the fear of catching COVID-19 on mental health in undergraduate students: a predictive model for anxiety, depression, and insomnia. Curr Psychol 2022 Jan 13;[Epub]. https://doi.org/10.1007/s12144-021-02542-5.
20. Kim K, Kim H, Lee J, Cho IK, Ahn MH, Son KY, et al. Functional impairments in the mental health, depression and anxiety related to the viral epidemic, and disruption in healthcare service utilization among cancer patients in the COVID-19 pandemic era. Cancer Res Treat 2021 Sep 17;[Epub]. https://doi.org/10.4143/crt.2021.585.
21. Okajima I, Chung S, Suh S. Validation of the Japanese version of Stress and Anxiety to Viral Epidemics-9 (SAVE-9) and relationship among stress, insomnia, anxiety, and depression in healthcare workers exposed to coronavirus disease 2019. Sleep Med 2021;84:397-402.
22. Cox RC, Olatunji BO. Linking insomnia and OCD symptoms during the coronavirus pandemic: examination of prospective associations. J Anxiety Disord 2021;77:102341.
23. Nami M, Mehrabi S, Kamali AM, Kazemiha M, Carvalho J, Derman S, et al. A new hypothesis on anxiety, sleep insufficiency, and viral infections; reciprocal links to consider in today’s “world vs. COVID-19” endeavors. Front Psychiatry 2020;11:585893.
24. Lee SA. Coronavirus anxiety scale: a brief mental health screener for COVID-19 related anxiety. Death Stud 2020;44:393-401.
25. Choi E, Lee J, Lee SA. Validation of the Korean version of the obsession with COVID-19 scale and the coronavirus anxiety scale. Death Stud 2022;46:608-14.
26. Lee SA, Jobe MC, Mathis AA, Gibbons JA. Incremental validity of coronaphobia: coronavirus anxiety explains depression, generalized anxiety, and death anxiety. J Anxiety Disord 2020;74:102268.
27. Kim C, Ahmed O, Park CHK, Chung S. Validation of the Korean version of the coronavirus reassurance-seeking behaviors scale during the COVID-19 pandemic. Psychiatry Investig 2022;19:411-417.
28. Ahorsu DK, Lin CY, Imani V, Saffari M, Griffiths MD, Pakpour AH. The fear of COVID-19 scale: development and initial validation. Int J Ment Health Addict 2022;20:1537-1545.
29. Hwang KS, Choi HJ, Yang CM, Hong J, Lee HJ, Park MC, et al. The Korean version of fear of COVID-19 scale: psychometric validation in the Korean population. Psychiatry Investig 2021;18:332-9.
30. Morin CM, Belleville G, Bélanger L, Ivers H. The Insomnia Severity Index: psychometric indicators to detect insomnia cases and evaluate treatment response. Sleep 2011;34:601-8.
31. Cho YW, Song ML, Morin CM. Validation of a Korean version of the insomnia severity index. J Clin Neurol 2014;10:210-5.
32. Lee J, Cho IK, Lee D, Kim K, Ahn MH, Chung S. Mediating effects of reassurance-seeking behavior or obsession with COVID-19 on the association between intolerance of uncertainty and viral anxiety among healthcare workers in Korea. J Korean Med Sci 2022;37:e157.
33. Lee SA, Crunk EA. Fear and psychopathology during the COVID-19 crisis: neuroticism, hypochondriasis, reassurance-seeking, and coronaphobia as fear factors. Omega (Westport) 2022;85:483-96.
34. Zheng Z, Peng F, Xu B, Zhao J, Liu H, Peng J, et al. Risk factors of critical & mortal COVID-19 cases: a systematic literature review and meta-analysis. J Infect 2020;81:e16-25.
35. Voitsidis P, Gliatas I, Bairachtari V, Papadopoulou K, Papageorgiou G, Parlapani E, et al. Insomnia during the COVID-19 pandemic in a Greek population. Psychiatry Res 2020;289:113076.
36. Li Y, Qin Q, Sun Q, Sanford LD, Vgontzas AN, Tang X. Insomnia and psychological reactions during the COVID-19 outbreak in China. J Clin Sleep Med 2020;16:1417-8.
37. Kokou-Kpolou CK, Megalakaki O, Laimou D, Kousouri M. Insomnia during COVID-19 pandemic and lockdown: prevalence, severity, and associated risk factors in French population. Psychiatry Res 2020;290:113128.
Fig. 1.Mediation model showing that the effect of coronavirus reassurance-seeking behavior or viral anxiety (independent variables) on preoccupation with coronavirus (outcome) is mediated by insomnia (mediator). e1, e2: error term. *Standardized estimator, p < 0.01. 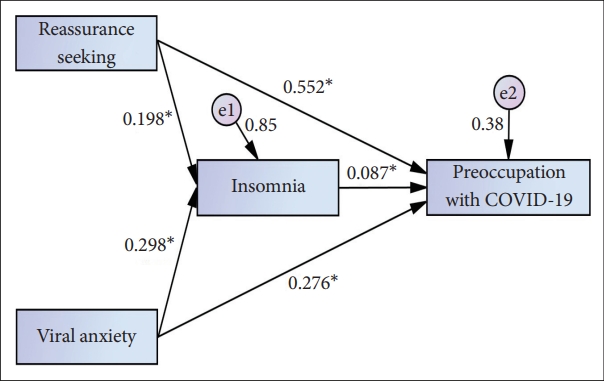
Table 1.Clinical characteristics of the study subjects (n = 400) Table 2.Correlation coefficients of each variable in all participants
Table 3.Linear regression analysis expecting preoccupation with COVID-19
Table 4.The results of direct, indirect, and total effects on mediation analysis |
|
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||